Anyone who’s torn their ACL can tell you how traumatic, painful, and life-changing the injury can be — and the recovery process certainly isn’t an easy one.
Typical recovery from ACL reconstruction surgery can take up to 9-12 months, although many athletes continue working on biomechanical movement errors for up to 18 months. As you can imagine, the physical and mental struggles of recovery can easily stir up feelings of uncertainty, especially over such a long span of time.
And, because you’re here, there’s a good chance you’re looking for information that’ll ease some of that doubt and worry.
Well, look no further — we’ve created a comprehensive timeline of ACL rehabilitation for you to reference through your own healing journey. Through this series of blogs, we’ll be detailing the typical protocol, healing times, and expectations for complete recovery all the way through returning to full activity. Each individual blog will cover a different month of the rehab process, allowing you to read up on objective recovery information as well as some examples from real-life ACL clients.
This first blog starts at “month 0,” or immediately after sustaining the injury. Most people will refer to this phase as the pre-rehabilitation phase, or “prehab” for short — but don’t worry if you haven’t heard of it before. That’s what we’re here for.
First Week After ACL Injury
Before you even get started with this whole prehab business, there are a few steps you need to take just within that first week of injury. You’ll have to follow several precautionary measures to help lessen your overall pain and reduce the chances of worsening the injury.

- Decrease edema and swelling — immediately after the mechanism of injury, you’ll start to experience a swelling known as edema around the knee joint. Although this inflammation is initially helpful for protecting your knee and preventing further injury, it can cause pain that limits your walking and joint loading. To help reduce this swelling, defer to the classic RICE method: rest, ice, compression, and elevation.
- Protect your knee — on top of the pain, you’re also likely to experience decreased range of motion and possible knee instability. Use a brace, ace wrap, or crutches to provide additional support for your vulnerable joint. (You’ll likely be given crutches to alleviate the loading on your knee, though the recommendation can vary based on your comfort, knee control, and daily movement demands.) In particular, stabilization braces are especially helpful for added security if you find yourself navigating busy environments.
- Meet with an orthopedic surgeon — this is where the science kicks in. When you meet with a surgeon for details on your injury, you’ll go through a full evaluation, MRI, and consultation. That sounds like a lot, and it may initially feel overwhelming, but all of this will provide you with more insight into what the rehabilitation process will look like for your specific injury. (Plus, the surgery itself isn’t always necessary; but more on that later.)
- Meet with a physical therapist — after speaking with a surgeon, you’ll want to seek a knowledgeable physical therapist to guide you through that “prehab” process. Because an ACL tear requires a lengthy timeline for full recovery, it’s vital to seek the help of a professional as soon as possible to ensure that your body is well prepared to take on the taxing nature of surgery and rehabilitation. Plus, since they’ll see you through your recovery, you’ll have a trusted person to turn to for expert guidance.
- Educate yourself — just like you are right now (give yourself a pat on the back)! There are plenty of credible resources for you to read up on, particularly regarding surgery, healing times, and rehabilitation demands. Although you’ll have reliable information from both your surgeon and physical therapist, it can be reassuring to self-educate and ensure that you aren’t overwhelmed by or unprepared for all the new oncoming procedures. Doing your own research can also help you realize what kind of questions you can bring to your surgeon / physical therapist, allowing you to seek direct answers and quell some of those uncertainties.
- Consider your athletic goals — the recovery process is a lengthy healing journey, so you’ll also want to refocus and mentally prepare for a new type of training. Your work will be geared more towards rehabilitation and recovery, rather than performance, so it’s important to understand what end goal you’re striving for. That being said, with your long-term goals in mind, make sure you’re focused on healing before improvement.
That can feel like a lot to take on within just one week, so don’t stress if you can’t get them all done right away. Some tasks are more easily accessible than others, so it’s reasonable to need a bit of extra time to book appointments and seek professional help.
However, it’s still imperative that you aim for these objectives as soon as possible. Besides, chances are that if you’re an athlete with a torn ACL, you’re already aching to get back to the sport. So why not get started on your healing journey right away?
2-4 Weeks After ACL Injury
By your second week after injury, you’re likely to experience less knee pain and more confidence in walking. All that icing, elevation, and rest has helped to diminish painful edema, which allows you to sleep more comfortably and stand for longer periods of time without pain.
If you didn’t get the chance to meet with an orthopedic surgeon in your first week, you’re most likely meeting with someone in week two. This can actually be an optimal time to schedule your MRI, as the scan will be easier to examine without the inflammation blocking the injury.
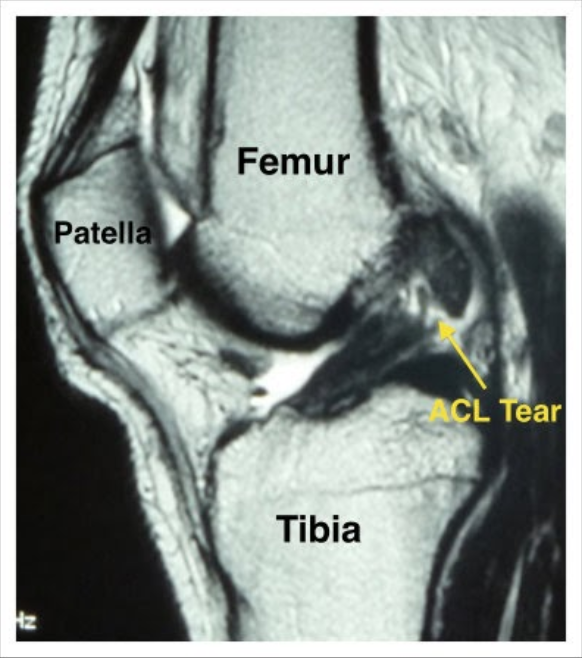
Similarly, your second week will likely be when you attend your first pre-operative physical therapy session. This first PT appointment will help evaluate the following aspects:
- Swelling reduction
- Pain levels and pain management
- Necessity for crutches, braces, or any additional compensation
- Range of motion
- Ability to squeeze your quadricep muscles
- Ability to squeeze and utilize your hip muscles
- Rehabilitation goals and sport participation
While evaluating each of these factors, your physical therapist will likely perform a gait assessment and prompt further discussion to understand your comfort levels and specific goals. Typically, by the end of your first session, you will have received some hands-on therapy to reduce swelling and improve your range of motion, as well as an at-home program that will help address balance, muscle activation, and functional movement.
While your first physical therapy session is designed to evaluate your functional status, your subsequent sessions over the next 2-4 weeks will focus on preparing your ACL for surgery and beyond — and that’s where the prehab process kicks in.
Prehabilitation Goals
Alright, let’s address the elephant in the room: what exactly is this prehab we keep talking about?
Well, in short, prehab is essentially the process of ensuring you’re both physically and mentally prepared to take on the road to recovery, particularly if it involves a surgical procedure.
The term itself may be relatively unknown to the general population, but the practice has become more common in physical therapy and medical settings over the last 5-10 years. In fact, the increase of prehabilitation techniques has been associated with the benefits of pre-operative training, particularly for helping restore patients’ functional capabilities before surgery.

For prehabilitation specific to the ACL, you’ll usually focus on the following objectives:
- Decrease edema and swelling — just as you did immediately after injury, continue to practice the RICE method to further reduce any lingering edema. Your physical therapist will likely perform therapeutic techniques to help lessen the swelling, as well. Through prehab, you’ll ideally be able to eliminate a majority of this painful swelling.
- Restore full, non-weight bearing range of motion (ROM) — this is one of the most important aspects to work on before heading into surgery. It’s extremely common for swelling or pain to limit your ROM after surgery, which can make it super difficult to regain full knee extension during post-surgical rehab. But, by regaining as much ROM as possible during prehab, you give yourself a headstart on rehab after surgery. It may sound weird, but your ROM before surgery is indicative of your postoperative ROM.
- Activate and maintain quadriceps strength — after an ACL injury, your quadriceps muscles will often experience some atrophy as a result of disuse and excessive swelling. This causes weakness in the muscle, which interferes with your natural gait pattern. If your quadriceps aren’t strong enough, your knees are less capable of bending or absorbing shock properly, which will prove detrimental to your recovery process. During prehab, it’s necessary for you to improve your quadricep strength, restore your natural gait, and improve your neuromuscular control.
- Maintain gluteus strength — similarly, your glute muscles need some love during your prehab, too. This is important to prevent your muscles from weakening, but research also indicates how proper strength and control of your gluteal muscles can help prevent future non-contact ACL injury.
- Restore balanced gait mechanics — sustaining a knee injury often causes people to avoid putting too much weight on the injured joint. While this is a natural (and often subconscious) reaction, walking with a limp can actually impede the functionality of your gait and slow your progress towards recovery. Walking with a limp is known as quadriceps avoidance walking, which is what it sounds like: walking in a way that avoids using that vital quadricep muscle. So, right in line with keeping that muscle properly strengthened and activated, your prehab will focus on restoring your usual walking gait so you no longer rely on limping.
- Maintain proprioceptive awareness — that sounds like a mouthful, but it basically just means practicing and improving the balance and control of your injured leg. Research has shown how proprioceptive training can decrease the risk of knee and ACL injury by about 95%, which are odds that you just can’t pass up.
- Continue educating yourself — as you progress through prehab, you’ll be moving closer and closer to that surgery date, so it’s helpful to look into postoperative resources. Focus on educating yourself on wound care and postoperative exercises to mentally prepare yourself; even if you expected this process from the get-go, undergoing surgery is a mentally taxing procedure that can cause a lot of uncertainty. It never hurts to give yourself a solid foundation of knowledge before diving into the process.
Now, we know that’s a lot to take in, but it’s more overwhelming in writing than it is in practice. All of this will be introduced gradually into your prehab training and guided by medical professionals, so there’s no rush to check off all the boxes right away.
Plus, keep in mind that recent research has continued to support the benefits of prehab: for many patients, practicing up to 5 weeks of prehabilitation improved their knee function, quadriceps peak torque, and total ACL work. So, now that you know the gist of prehab and all its benefits, it’ll hopefully feel more approachable as you take on this beast of a recovery process.
Week 4 and Beyond (Do You Need Surgery?)
After completing 4 weeks of prehab, you’ll start to notice improved confidence in your ability to walk, squat, and perform other basic movements. And that’s pretty impressive for only about a month, right?
By this point, most people don’t experience any more knee pain (unless they had an additional injury to their knee, like a meniscus tear). As a result, many patients end up wondering if they even need surgery anymore, since most of the surface-level symptoms have already been alleviated.
And it’s a fair question — but one with a complicated answer.
Although it’s an extremely common procedure for many, seeking surgical treatment isn’t always a necessity for athletes.
In order to determine whether or not it’s absolutely necessary, you’ll likely go through an evaluation depending on your sport, athletic goals, and level of play. Determining whether or not to have surgery is largely based on an athlete’s pre-injury function and future goals, rather than immediate objective measures.
For those who aren’t interested in returning to sports, or for those who perform sports with low levels of cutting and jumping (like cycling), you have the option to avoid surgery. There’s growing evidence that shows how individuals with a stable knee following ACL injury can rehabilitate to a functional level without surgery — it just depends on how you define “functional level.”
This non-surgical approach, however, is thought to be most useful for older individuals who have a better grasp of their activity levels and very little demand for movements like cutting or changing direction. For younger individuals, surgery is usually a tougher decision, as it can be challenging to predict what kind of activities you may want to participate in later in life. In this case, you’ll likely require further discussion before coming to a decision.
However, for athletes who wish to maintain their active lifestyle, surgery is still the best option to properly stabilize the knee joint. Even if your prehab has allowed you to function pain-free during your daily tasks, that isn’t the whole picture — most everyday tasks require minimal lateral or twisting movements, therefore placing very little strain on your knee ligaments, so it makes sense to feel little to no pain.
But if you were to get back to performing activities that involve sprinting, cutting, jumping on one leg, or changing direction, you definitely wouldn’t be at peak performance. You’d likely notice weakness or decreased stability, potentially causing you to fear movement or reinjury — meaning it’s still way too early for your body to take on the regular demands of your sport. Typically, most high school, collegiate, and professional athletes will undergo ACL reconstruction very soon after injury to preserve valuable post-operative time. (After all, the longer you wait, the longer you’ll be out of your sport for the coming year.)
At this point in your prehab, you should speak with your surgeon to determine a surgery date, as most ACL surgeries are performed somewhere between 2-6 weeks after the initial injury. Your physical therapist will send over a progress report highlighting your objective measures, so the surgeon will have a full understanding of your pre-operative function before setting a date.
Final Thoughts for Prehabilitation
If you’ve sustained an ACL tear and want the best outcome, it’s imperative that you start your recovery immediately after injury. Not only should you take proactive steps to lessen your pain, but also to ensure that you team up with resources and experts that’ll provide you with the best guidance for proper healing. Make sure you discuss prehabilitation with your surgeon, especially when considering surgery, and adhere to the necessary physical therapy training to ensure optimal postoperative results.
Once you’re through the surgery, you’ll move into the first month of post-op work. Check out the next blog of our series, where we’ll discuss the goals, trials, and psychological factors associated with the first month out of ACL surgery.
But, in the meantime, take care of that prehab — you got this.

